Most healthcare providers know what a Megacode is. Fewer understand what the 2025 American Heart Association guidelines changed about how one should be run — and why those changes matter in the room where your team actually works.
The AHA released its most significant update to CPR and Emergency Cardiovascular Care guidelines on October 22, 2025. These revisions are in effect through 2030 and represent the most current standard of care for every ACLS provider in the country. If your team was certified before October 2025, there are clinical details in this post that may differ from what you were taught. Read carefully.
This guide covers the seven core ACLS Megacode scenarios, the key 2025 guideline changes that affect each one, and what genuine Megacode preparation looks like beyond checking a certification box.
What an ACLS Megacode Actually Tests
An ACLS Megacode is a timed, team-based simulation of a real cardiac emergency. It is not a written test, and it is not a multiple-choice quiz. It places a provider — or a team of providers — in a scenario that closely mirrors what happens in a real code: a patient deteriorating in front of you, a monitor showing a rhythm that demands a decision, a crash cart that needs to be opened, and a team that needs to be led.
What instructors evaluate in a Megacode goes well beyond whether you know the algorithm. They assess whether you can apply the algorithm under pressure, communicate clearly to a team that is simultaneously performing compressions, managing an airway, and establishing IV access, and make correct decisions in the precise sequence the patient's condition requires.
The 2025 guidelines place heightened emphasis on human factors — closed-loop communication, transparent role assignment, and coordinated team performance — as measurable components of resuscitation quality. Nearly half of resuscitation errors are attributable to communication and leadership failures, not clinical knowledge gaps. The Megacode now explicitly tests for both.
The 2025 Unified Chain of Survival
One of the most significant structural changes in the 2025 guidelines is the consolidation of the Chain of Survival into a single, unified framework covering adult and pediatric, in-hospital and out-of-hospital cardiac arrest. Previously, different chains existed for different settings. The 2025 update standardizes the model so every provider — regardless of setting — operates from the same mental framework.
This matters for Megacode preparation because it aligns the cognitive model you use during training with the one you will use in a real emergency, regardless of whether that emergency occurs in an ICU, an urgent care, a dialysis center, or a patient's home.
7 ACLS Megacode Scenarios: 2025 Standards
1. Ventricular Fibrillation (V-Fib) and Pulseless Ventricular Tachycardia (pVT)
V-Fib and pulseless VT remain the highest-priority shockable rhythms in ACLS. The 2025 algorithm preserves the familiar structure — high-quality CPR, defibrillation, 2-minute cycles — but sharpens several clinical details that providers need to know.
- What changed in 2025: The guidelines now explicitly prioritize IV access for drug delivery over intraosseous (IO) access. IO remains a reasonable option when IV cannot be obtained quickly without delaying key interventions, but the language is clear: IV first.
- Epinephrine remains the standard vasopressor — and in 2025, it is the only vasopressor in the cardiac arrest algorithm. The routine administration of sodium bicarbonate, calcium, magnesium, or steroids in undifferentiated cardiac arrest is explicitly not recommended unless a specific indication exists.
- Amiodarone and lidocaine remain acceptable antiarrhythmics for refractory VF/pVT. The 2025 guidelines present them as reasonable alternatives.
- Waveform capnography is reinforced as the standard for monitoring CPR quality and detecting return of spontaneous circulation (ROSC).
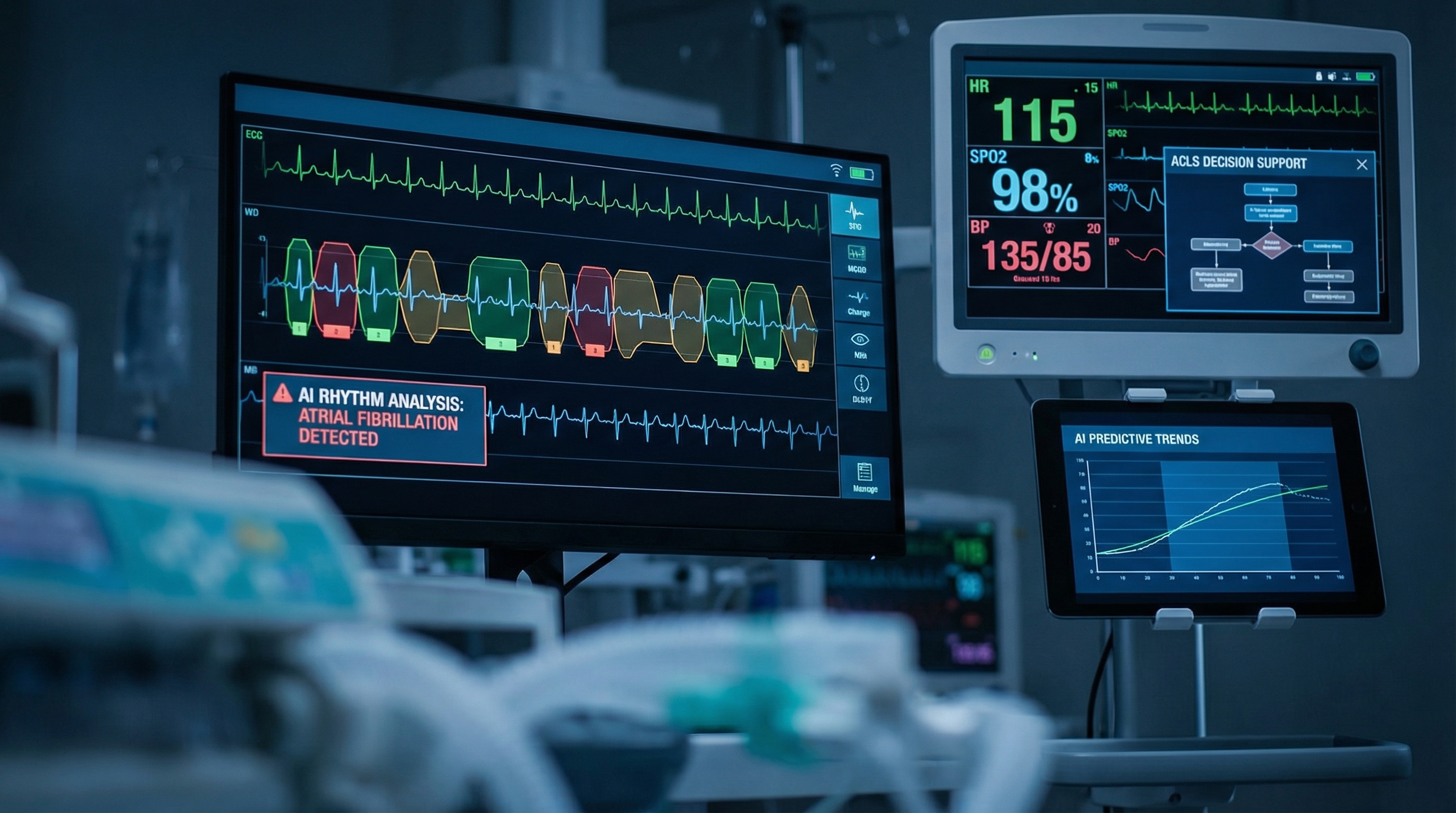
2. Pulseless Electrical Activity (PEA) and Asystole
PEA is the scenario that exposes the difference between a provider who has memorized an algorithm and one who actually understands resuscitation. The monitor shows organized electrical activity. There is no pulse. The team must maintain CPR, administer epinephrine, and simultaneously work through the reversible causes — the H's and T's.
What changed in 2025: The post-cardiac arrest care pathway following ROSC in PEA has been deepened significantly. The 2025 guidelines treat post-arrest care as a continuation of resuscitation, not a handoff. Updated parameters include tighter guidance on oxygenation targets, blood pressure targets, temperature management strategy, and neurologic assessment protocols.
The H's: Hypovolemia, Hypoxia, Hydrogen ion (acidosis), Hypo/hyperkalemia, Hypothermia, Hypoglycemia.
The T's: Tension pneumothorax, Tamponade (cardiac), Toxins, Thrombosis (pulmonary), Thrombosis (coronary/STEMI).
3. Tachycardia — Unstable and Stable
Tachycardia management in ACLS requires the provider to make a critical binary decision before any treatment: is this patient stable or unstable? The answer determines everything that follows.
An unstable tachycardia requires immediate synchronized cardioversion. This is not a medication-first situation. The 2025 guidelines sharpen the emphasis on this decision point, reinforcing that unstable patients should not receive drug trials before electrical therapy.
4. Bradycardia With a Pulse
Symptomatic bradycardia is managed based on clinical presentation, not heart rate alone. The 2025 guidelines reinforce that treatment is driven by symptoms and perfusion status.
What changed in 2025: Atropine dosing is confirmed at 1 mg IV bolus, repeated every 3–5 minutes to a maximum of 3 mg. The older 0.5 mg dosing has been definitively replaced. Dopamine infusion is reaffirmed at 5–20 mcg/kg/min.
5. Stroke
Stroke is included in ACLS because rapid recognition and the first-hour response directly determine whether a patient has access to time-sensitive interventions. Every minute of untreated ischemic stroke results in the loss of approximately 1.9 million neurons.
The Cincinnati Prehospital Stroke Scale (FAST — Face, Arms, Speech, Time) remains the primary recognition tool. Time of last known well, not time of symptom recognition, is the critical clock that governs treatment eligibility.
6. STEMI — ST-Elevation Myocardial Infarction
STEMI represents complete occlusion of a coronary artery with ongoing myocardial ischemia. Door-to-balloon time (for primary PCI) is the metric that determines outcome.
2025 clinical priorities: Recognize the STEMI ECG pattern. Initiate dual antiplatelet therapy. Activate the Cath Lab. Manage pain, anxiety, and oxygen appropriately — noting that supplemental oxygen is indicated only when SpO₂ is below 90%.
7. Respiratory Arrest and Opioid-Associated Emergencies
The 2025 AHA guidelines made a significant structural addition by explicitly incorporating naloxone into the algorithm for suspected opioid-associated cardiac arrest and respiratory arrest.
What changed in 2025: Naloxone is now explicitly positioned in the algorithm for respiratory arrest in the context of suspected opioid overdose. If a pulse is present but the patient is not breathing adequately, rescue breathing and naloxone administration are the first-line response.
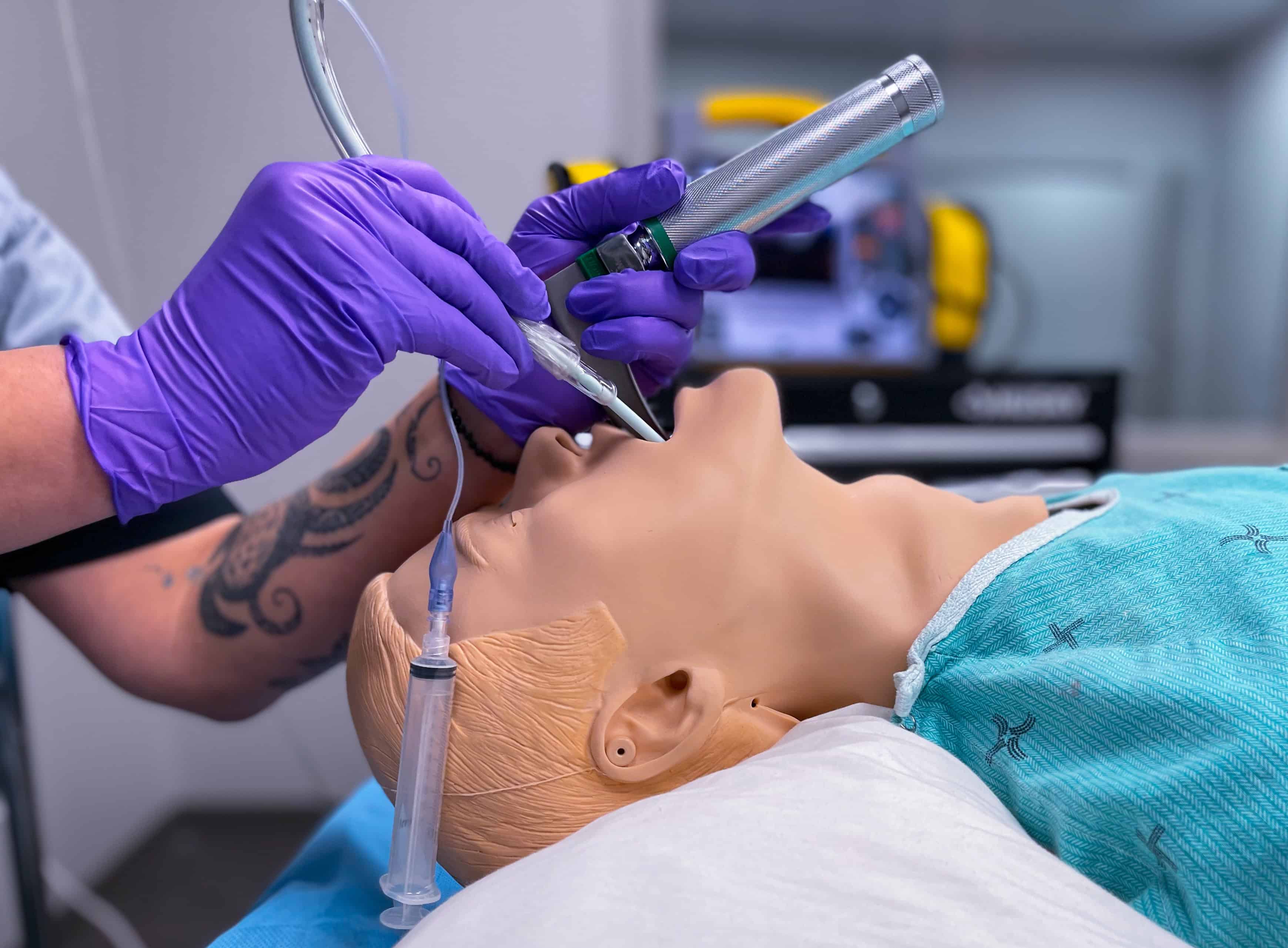
Key Components of Every Megacode: 2025 Standards
- Initial Assessment: High-quality compressions (100–120/min, at least 2 inches depth, full recoil, minimized interruptions) must be maintained throughout code.
- Waveform Capnography: The 2025 guidelines reinforce ETCO₂ monitoring for real-time CPR quality assessment and ROSC detection.
- Airway Management: Bag-mask ventilation remains the first-line airway intervention. Advanced airway placement is appropriate when prolonged resuscitation makes continuous bag-mask ventilation impractical.
- Medication Administration: IV access is prioritized. IO is the backup.
- Team Communication: Closed-loop communication is a measurable resuscitation competency.
- Post-Resuscitation Care: ROSC is not the finish line. The team leader is expected to have a post-ROSC plan ready before ROSC is achieved.
Megacode Team Roles
Every position in a Megacode team is an evaluated role:
- Team Leader: Directs the resuscitation, makes clinical decisions, maintains situational awareness.
- Compressor: Delivers high-quality CPR and calls for rotation at the 2-minute mark.
- Airway Manager: Maintains patent airway, delivers ventilations.
- IV/IO and Medication Nurse: Establishes access and administers medications.
- Monitor/Defibrillator Operator: Interprets rhythms, charges and clears for defibrillation.
- Recorder/Timer: Tracks CPR cycles, medication timing, and clinical events.
What Separates a Prepared Team From a Certified One
A passed Megacode means the provider demonstrated minimum competency in a controlled setting. A prepared team means the skills are automatic enough to survive the additional cognitive load of a real emergency.
The 2025 AHA guidelines are not just a list of clinical updates. They represent a framework for resuscitation that is more precise, more team-centered, and more demanding than the 2020 guidelines they replace.
Train to the 2025 Standard on the Treasure Coast
At Finish Strong CPR & Medical Training, every ACLS course we teach reflects the current 2025 AHA guidelines. We offer same-day ACLS certification with digital eCard issuance on completion, on-site group training for clinical teams across Martin County and St. Lucie County, and a managed renewal calendar so your team is never caught with an expired card.
Confident Teams. Compliant Workplaces.
Schedule Your Certification TodayThis content reflects highlights from the American Heart Association's 2025 CPR & ECC Guidelines, released October 22, 2025. For complete official recommendations, visit cpr.heart.org. Finish Strong CPR & Medical Training is an independent multi-certified training organization and is not affiliated with or endorsed by the American Heart Association.

